A few months back, I wrote an in-depth piece about histamine intolerances. New research suggests that it may be causing symptoms that seem to be coming from completely different causes including gluten sensitivity.
Is Histamine Intolerance Real?
There is clear data indicating that histamine from foods can be absorbed. This can cause troubling symptoms that go beyond nocebo reactions.1
Furthermore, histamine intolerance has a history of being underdiagnosed. There are those who have had it, and suffered from symptoms, with no concrete explanation for them.
Key Insight: Many symptoms that come alongside histamine intolerance are vague. With no tests able to rule it out, it can often be overdiagnosed or misdiagnosed.
Histamine Intolerance?
The first thing that I would say is that I think the term “histamine intolerance” is an improper phrase. It can be very misleading because it is definitely not an intolerance to histamine. It is not an allergy or an autoimmune response against histamine (even if it sounds like it).
Histamine is a normal part of our bodies. To date, no humans have been documented as being intolerant or allergic to histamine. So, I think that this term really gives an unclear first impression for those trying to learn.

Bottom Line: The body forms histamine as an important part of brain cell communication and immune regulation. This normal part of our body is not something that we should fear. Instead, we should be more concerned about the level of it (rather than its presence).
What Are The Specific Symptoms?

When we think of symptoms involved with this overload of histamine, we primarily look at some of the classic “allergy” symptoms. These include:
- Insomnia
- Dizziness
- Anxiety
- IBS
- Rashes
- Skin flushing
- Palpitations
- Headaches
- Fatigue
- Edema
- Sinus congestion
These are classic symptoms. You could take any one person, give them a mega dose of histamine, and they will start developing them. It is bound to happen, and most importantly of all, they can be life-threatening.
Bottom Line: It is not that people are “intolerant” of histamine, instead they simply have too much of it. They have more than they need circulating throughout their body, and that is where these symptoms take root.
What Are The Vague Symptoms?
Remember when I mentioned that one of the tricks of histamine intolerance is that symptoms are often present? A lot of these vague symptoms can be born from chronic, elevated levels of histamine.
This is where things get murky, but here is what one could expect:
- Changes to the menstrual cycle
- Generalized fatigue
- Headaches and migraines
- Difficulty sleeping
- Having a hard time waking
- Struggling to feel energized
- High blood pressure
- Vertigo and dizziness
- Cardiac palpitations
- Poor regulation of body temperature
- Anxiety, nausea, vomiting, and cramps
Bottom Line: These are all possible symptoms that can be associated with histamine intolerance. It does not mean that they are definitely going to happen – only a possibility. Because they are so general, it is difficult for us to think of them too specifically.
Why Would Someone Have Too Much?
This goes back to the idea that histamine intolerance is less of being intolerant, and more of having an overload. How would someone end up with more histamine than they need?
Think about it like this: your body has histamine coming in, and histamine going out. These are the main two things that your body is in charge of.
From there, two issues can arise: too much coming in or too little coming out. There would have to be a deficiency on one end and that typically starts with the amount taken.
Let’s pull back some more, and start from the beginning. When we think about histamine, we can understand it as a natural response to:
- An allergy
- A chronic infection
- Some sort of chemical trauma to your body
Histamine leaves your body by way of various enzymes in your body that are in charge of breaking down histamine in your body.
Histamine is known as a biogenic amine, which means that it triggers an inflammatory response in your body to make this happen.
Key Insight: The problem is that you could easily have too many of these being made, and not enough being unloaded. The former is more likely, and the latter (due to gene defects) is quite rare.
Understanding DAO Deficiency
A DAO deficiency is what we might understand as the gene defect which makes it difficult for your body to “unload” histamine from your body. This is what may cause histamine overload, triggering all those nasty symptoms previously mentioned.
While they are possible, they are not very probable. From the populations that I have seen, from people who think that they have a lack in that ability, I would argue that it is being overly-suspected and overdiagnosed.
One of the reasons why is because all of those symptoms, the vague ones, could be attributed to many other conditions.
The thing about the DAO deficiencies is that they are completely measurable. You can take a test and find out if you have it.
Key Insight: When it comes to high histamine in the blood, you might be able to see it present, but you cannot always see it present – even if it is happening. That is where things get difficult and cause a lot of issues.
What it takes is a lot of judgment, and there is no standard answer that satisfies people across all situations. It is just not that easy.
The thing is that when you are entertaining a diagnosis that you cannot objectively affirm in some way, you have to tread very lightly.
The last thing you want to do is settle on an answer when you are misattributing symptoms that are coming from another cause altogether.
Bottom Line: There could be something different, and unrelated, causing the exact same symptoms that you might have thought were being caused by histamine intolerance.
Stress & Anxiety
There are even instances where the other symptoms, like hives and flushing, can come from stress and anxiety.
One can have very real physical symptoms, but misattribute them to a genetic defect (as opposed to something like generalized anxiety).
In the end, these things cut both ways. There are many that do have these problems that remain undiagnosed, and there are others who fall in the overdiagnosed camp.
Reading yourself into three or four symptoms does not mean that you can jump to conclusions, and it always helps to test – suspend judgment, until you know the whole story.
How do you diagnose histamine intolerance?

First, you can do it empirically. What that means is that if you take histamine blockers, and feel better, it is not unreasonable to think that histamine intolerance was the root of the problem.
The difficulty here is that histamines have a great deal of influence on your body. It can affect your:
- Overall mood
- State of anxiety
- Stress or panic levels
These are all things that histamines effect, and that histamines lower! This all goes back to the fact that things like anxiety can trigger responses like rashes, and in taking an antihistamine we can sedate ourselves and feel better (and less anxious).
Even though anxiety was our overall issue, we might attribute it to a histamine intolerance instead.
The other difficulty with histamine has to do with its production in the body. Your body makes histamine in response to allergies, infections, stress, or trauma, but we also do get it from some foods in our diet.
Certain bacterial events can even make the amine levels in foods lethal and have caused issues in the past. This thinking, though, has led people to believe that the levels of histamines in certain foods can act as a trigger.

Key Insight: While it is plausible, there have been many studies looking at quantifying the level of histamines in foods. These studies, after all their research, and in no way in agreement over what constitutes a “high-histamine food.”
Trends in Foods
Even though we have no data on specific foods, some trends have emerged about foods that are higher in histamines:
- Cured or smoked meats
- Aged cheeses
- Fermented foods
- Shellfish
These are categories of food that have been known to be higher in histamines. Does this mean you should avoid them?
Well, if they clearly cause symptoms they could be relevant. But, I really cannot endorse any sort of “histamine food list” because there are just way too many contradictions. The science is just not there yet.
For that reason, I would also not recommend diets that are designed to cut down on histamine ingestion just yet.
Due to the fact that there is so much conjecture around what constitutes a “high-histamine food,” if you went on a low-histamine diet you would be cutting out a lot of food. You might not be doing your body any good.
Otherwise, we might look to things like DAO replacement compounds (which you can take in pills), or mast cell stabilizing compounds (which are quite high in bioflavonoids).
The cycle is that when mast cells are more stable, and less likely to “pop open” with histamine, you are simply less likely to get symptoms.
Bottom Line: Whether it comes from your diet or from other compounds, it is important to know that histamine intolerance might not be the end of the story. While it might make you feel better, it is just as important to know the root cause of whatever issues you are dealing with – because it might even be more than one.
Histamine Intolerance: The Latest Research
While updating this article, I found research that related to two key ideas as it pertains to histamine intolerance. They are:
- There is more information on histamine intolerance as a possible cause of non-celiac gluten sensitivity
- There is more data on histamine intolerance tests being valid (with new tests emerging)
Histamine Intolerance and Gluten Sensitivity
There are many people, without celiac disease, who have noticed an improvement in digestive symptoms when they follow a gluten-free diet.
While this is good for many reasons, the drawback is that for many people, gluten-free diets end up being lower in fiber and higher in processed fats (on top of being more expensive).2
Also quite prevalent in these discussions are that gluten-free diets lead to higher risks of diabetes and weight gain. Low-gluten diets may also be associated with a higher risk of type 2 diabetes.3
The truth is that most dietary gluten comes from:
- Bread
- Other baked goods
- Processed foods
- Pizza
- Beer
These same foods are also high in histamine, and they are quite often seasoned with high-histamine ingredients.
The symptoms of non-celiac gluten sensitivity are similar to those of histamine intolerance and are mediated by histamine receptors. These symptoms include:
- Bloating
- Gas
- Abdominal pain
- Reflux
- Nausea
- Vomiting
- Irregular bowels
- Constipation
- Fatigue
- Headaches
- Migraines
- Eczema
- Rash
- Dermatitis
- Hives
- Rhinitis
- Angioedema
Histamine Intolerance: Test
The mindset that I would encourage for histamine intolerance, and that I often encourage when it comes down to figuring out root causes for issues, is all about testing.
If you test and something is obviously there, it is worth treating and pursuing further.
On the other hand, if it is not there, consider a trial of lowering histamine (in terms of the obvious foods that we detailed earlier), and think about things that help stabilize your mast cells.
Since initially writing this article, some potentially useful tests have come to the fore which may help our conversation today. First is testing for diamine oxidase enzyme activity.
If low, it can be diagnostic, but it is not perfect as a test. It either misses many with histamine intolerance, or many with symptoms of histamine intolerance have some other underlying issue.4
Key Insight: The best test to date is likely a skin-prick test. It can accurately identify 79% of those with histamine intolerance.5
While our best bet right now is the skin prick, future new tests may be used to measure the amount of histamine and methylhistamine in urine.6
Also, please do look deep into any hidden infections, gut issues, airborne allergies, food intolerances (Read: The ultimate guide to food intolerances). Those are the more likely culprits and are certainly worth your time.
Bottom Line: If you continually “chase” the diagnosis of histamine intolerance, and it is not measurable in your body, you are playing a losing game. Even if you strongly suspect it, you will never know if you have gotten a handle on it. So, please, expand your perspective and try to treat these other issues – they could also be the root cause of your symptoms.
New Studies: 2018
What else have we learned in 2018 that we did not know before about histamine intolerance? Low-histamine (and not histamine-free) diets can help with chronic urticaria (hives).7
This is a hard condition to treat, with consistent causes to be found.
One study that showed that a low-histamine diet, one which could lower urticaria, avoided the following foods:
- Anchovies
- Sausage
- Ham
- Chicken
- Tuna
- Anchovy
- Shrimp
- Miso
- Spinach
- Kimchi
- Cheese
- Seaweed8
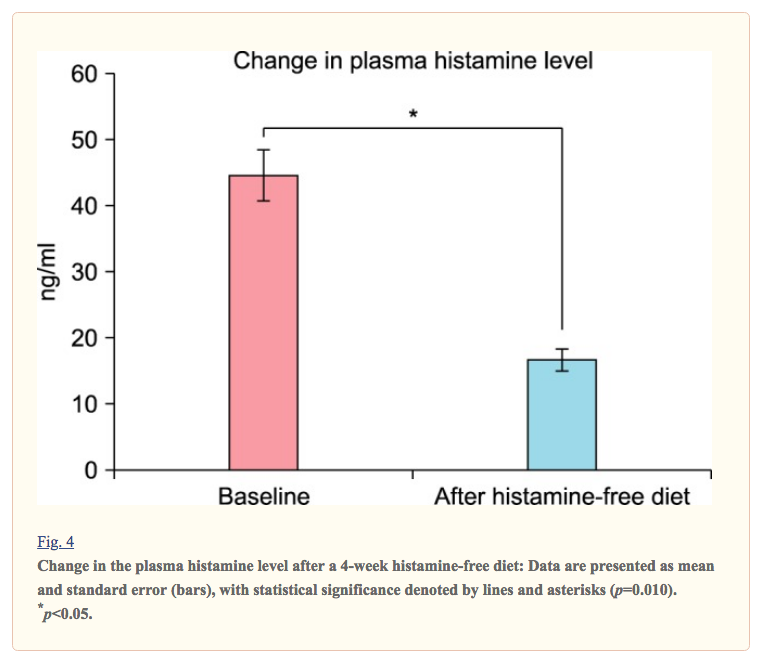
The diet itself lasted 4 weeks, with the symptoms improving and plasma histamine levels reduced overall. Lastly, DAO activity did not change.
The final study that I want to highlight surrounds DAO supplements. In a blinded study from 7 hours and 32 minutes to 6 hours 41 minutes – patients noted a reduction in migraines of 1 hour and 24 minutes.
In the study, the placebo reduced the duration of migraines by 54 minutes. While it seemed that they did help but in the final tally they reduced migraine duration by 6%.9

Updated Knowledge, Optimized Health
Now that we have learned a little bit more about histamine intolerance, and the latest research surrounding it, I want to help you learn even more about your body.
Please consider taking the Thyroid Quiz (Click Here) today.
It will give you a lot more information than you might have even thought possible and can put you on the right path to leading a healthier life.
Sources
1 – https://www.dropbox.com/s/kpkw3itr101e01e/10.1016%40j.aller.2016.04.015.pdf?dl=0
2 – https://www.ncbi.nlm.nih.gov/pubmed/26427614
3 – http://newsroom.heart.org/news/lowgluten-diets-may-be-associated-with-higher-risk-of-type2-diabetes?preview=b2db
4 – https://www.ncbi.nlm.nih.gov/pubmed/29154390
5 – https://www.ncbi.nlm.nih.gov/pubmed/23724226
6 – https://www.ncbi.nlm.nih.gov/pubmed/28715791
7 – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5839887/
8 – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5839887/#S1
9 – https://www.ncbi.nlm.nih.gov/pubmed/29475774

1. Schedule a Thyroid Second Opinion with me, Dr. C, Click Here for Details
2. Download and use my Favorite Recipes Cookbook Here
3. Check out my podcast Medical Myths, Legends, and Fairytales Here
Dr. Alan Glen Christianson (Dr. C) is a Naturopathic Endocrinologist and the author of The NY Times bestselling Adrenal Reset Diet, The Metabolism Reset Diet and The Thyroid Reset Diet.
Dr. C’s gift for figuring out what really works has helped hundreds of thousands of people reverse thyroid disease, lose weight, diabetes, and regain energy. Learn more about the surprising story that started his quest.


