Many people have been told that their pituitary gland makes their TSH and T3 levels unreliable. I want to explore more about what they asked, what it means, and what they (and what you) can do about it. Let’s talk more about your optimal T3 levels!

A Question From A Reader
I am always so excited when I receive questions from readers. It is nice whenever someone chooses to engage and to reach out in order to do what is best for their health. Please, if you or someone you know has a question, reach out!
This question, in particular, goes like this…
“I read your article on T3, and my functional doctor says it does not apply to me as I have a pituitary problem because my TSH is low and my T3 is low.”
Should you ignore your TSH, and take T3, because of your pituitary? This is a really good question and a concern that I am sure lots of people have. That’s why today I want to discuss it, explore some of the science, and what you can do moving forward.
Your T3 & Your Pituitary
The short answer to this question is that it is a common misunderstanding that I have seen all too often. Both in practice throughout the United States and even during my times in Mexico.
In situations like this one, it is extremely rare that the pituitary gland is the culprit behind thyroid disease. But, there are definitely some ways of knowing if it is likely or not.
There is a reason why it can look that way, specifically when your TSH and your T3 are both low.
How Could Your Pituitary Cause Thyroid Disease?
Let’s back up a bit. When your entire endocrine system is working properly, the hypothalamus is telling the pituitary to go to work. From there, the pituitary tells the thyroid to work. It would also tell the adrenals, the ovaries, and the testicles to do their jobs, too.
Interested in learning more about your thyroid levels? Let’s back up and start here…
Even if they could work faster than ever, if the pituitary does not tell them to work, they simply will not. At the same time, if the hypothalamus was not working, the pituitary would no longer tell anyone to do anything.
Key Insight: If the hypothalamus or the pituitary are not functioning properly, this is what we call central hypothyroidism.

The term “central hypothyroidism” comes from differentiating itself from what we also know as “primary hypothyroidism.”
Primary hypothyroidism is when the thyroid simply cannot work. This is when we might consider the thyroid to be the primary problem.
On the other hand, central hypothyroidism is when the thyroid is not working because it is not being told to work (and not because it cannot work on its own).
These are further broken down into two types:
- Secondary – When the pituitary fails to tell the thyroid to work.
- Tertiary – Where the hypothalamus fails to tell the pituitary to tell the thyroid to work.
Bottom Line: Our reader’s question from before sounds like they are describing a case of “secondary central hypothyroidism.” The pituitary is failing to tell the thyroid to work, and therefore the thyroid is unable to do its job properly (even if it is perfectly healthy).
How Common Is Central Hypothyroidism?
Amongst reported cases of hypothyroidism, about 1 case per every 80,000 – 100,000 instances of hypothyroidism is caused by a pituitary disease.
What does that mean? Well, it is really, really rare for you to be dealing with central secondary hypothyroidism.
Taking a step further back, there have only been about a dozen cases across the globe that have ever dealt with tertiary central hypothyroidism (instances where the hypothalamus is not operating properly). It is exceedingly rare.

What Causes Central Hypothyroidism?
The most common problem is where someone has a tumor on their pituitary gland. Those are what we call “space-occupying lesions.” They are lesions which take up space and do one of two things:
- Crush the pituitary to where it will no longer work.
- Grow to where the pituitary is asking every other gland to work too much.
Key Insight: By and large, pituitary disease deals with instances where things are either all turned on (in cases of growth). Or all off, in cases of squeezing the gland into oblivion. This affects everything, and not just the pituitary.
There are also cases wherein a growth, or what we know as an adenoma, can be found in one of two forms. You could have:
- A microadenoma
- A macroadenoma
Microadenoma is one that is relatively tiny, less than 14 millimeters. A macroadenoma is one that is larger than that 14 mm threshold. In general, macroadenomas are the ones that inspire large-scale hormonal changes to the thyroid or elsewhere.
These macroadenomas also tend to be large enough to where they squeeze on the nerves that go from the eyes to the processing centers that you have in the back of your brain. Therefore, your vision can also be distorted in cases of macroadenomas.
Bottom Line: If both your vision is distorted, and your hormones are way off, it could be a pituitary disease. It is rare, but it does happen.
Understanding Low T3 and Low TSH
So, what can we say is the more common result? If pituitary disease is that rare, there must be something more common that explains why both our T3 levels and our TSH scores are low. Here is what I have to tell you…
Much more commonly, doctors will look at lab results that have a low TSH, low T3 score and assume the pituitary is not working. The thought process is that if the pituitary was working correctly, that a low TSH would correspond with a high T3 level.
Do you depend on your thyroid? We all do. Do what’s right for it and start here…
The thyroid is being told to work by what we know as thyroid stimulating hormone (TSH). In cases where it is overactive, the pituitary lowers TSH on purpose. In order to try and balance out your thyroid and to get it working properly again. (Read: Should you ignore your TSH)
That is why a lot of doctors would look at a lab report with a low T3 and a low TSH, and start to scratch their heads and wonder what is going on. They are thinking, “if there is too little T3, why wouldn’t the pituitary tell the thyroid to work harder?”
From there, they assume the pituitary is to blame. The slide that I have shown below really illustrates what I am talking about here. Let’s take a look…
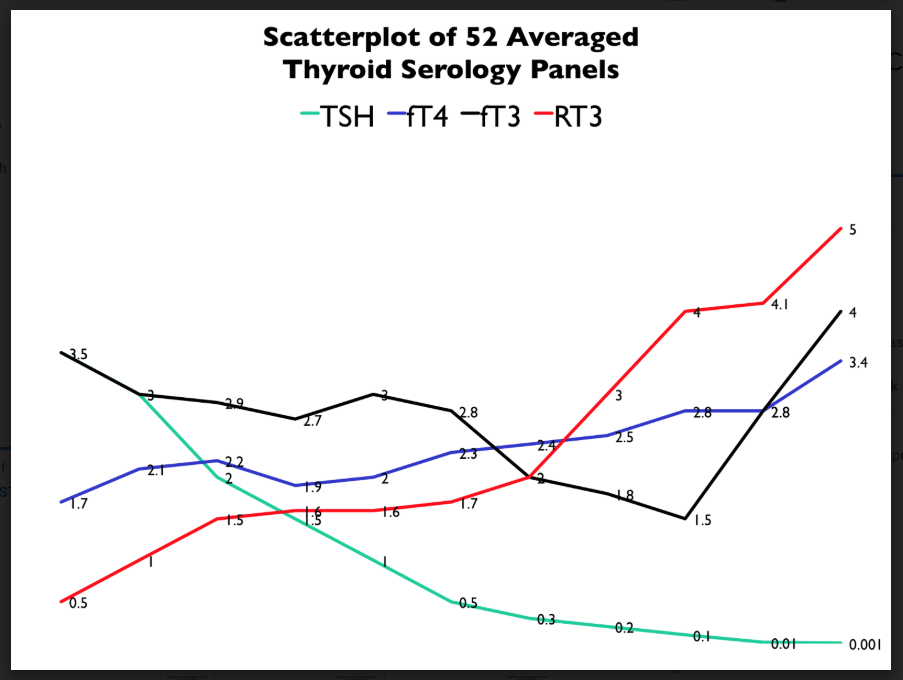
I generated this handy scatterplot from 52 different thyroid tests. These show how the TSH, the free T3, the free T4, and the reverse T3 tend to move together. What does it all mean, though?
What happens here is that the pituitary tells your body to produce more or less thyroid hormone (in fact, that your body needs it). Specifically, though, it is telling the thyroid whether or not it should get bigger or smaller.
When there is too much hormone, the pituitary lowers the TSH. This is what you can see on the right hand of this slide, in the form of the blue line making a downward trajectory.
When there is too little hormone, the pituitary demands more TSH. This is the opposite side where you can see that same blue line making a steady upward climb.
On the left side, where the black line (your T3) and the green line (your TSH) intersect, the T3 levels make a brief dip before raising up again (as your TSH drops). I really want to focus on what is happening right there, at that moment.
Basically, your brain is telling your thyroid how much hormone it wants. But, the rest of your body is trying to make due with the wrong amount of thyroid hormone currently in your system. So, as it dips, you may stop seeing these two correspond with one another.
At about 0.1 on this graph, both the T3 and the TSH has dropped. Your brain is basically telling your thyroid to slow down, all while your liver and your kidneys are bailing out this extra thyroid hormone that they think is the new normal.
Key Insight: Your body’s peripheral metabolism and regulation is helping out your pituitary.
We can see the same thing happening at the opposite end of this same graph. Patients can be getting hypothyroid and can be experiencing high levels (especially of T3, in particular). There is too little hormone, so the body is essentially stockpiling it for fear of losing more.
Bottom Line: It is really common to where someone is getting too much thyroid medication, or their body is over-producing thyroid, to where they have lower levels of both these hormones. Long story short, in almost every case, it is not a problem with the pituitary. In fact, it’s a completely normal response!
Action Steps: What You Can Do

Sadly, in a lot of these cases, what a doctor will want to do is simply prescribe more thyroid hormone. If they do, eventually the free T3 will go up, but only once the TSH has gone very low (which is not safe and basically equates to a thyroid overdose).
Key Insight: A thyroid overdose can cause a lot of risk to your brain, your heart, and your bones. I do not want that for you, which is why I want to provide you with some action steps that you can take when your doctor suspects you might be dealing with a pituitary disease.
If you are ever in a situation like this one, please know that pituitary disease is almost never the culprit (except in very, very rare cases). It can be, but it helps to be working with a doctor who specializes in endocrine diseases when you do seriously consider it.
What would a thorough diagnosis look like? It would involve a scan of your pituitary, as well as an understanding of all the pituitary hormones (not just the TSH, but FSH, LH, and ACTH).
Bottom Line: If a doctor does not diagnose it properly, then they cannot diagnose it as strictly a pituitary problem – and, therefore, they cannot ignore your TSH.
Understanding Your T3 Levels
I hope that I have helped both the reader who asked that previous question, as well as all of you, gain a better understanding if your pituitary is truly at the heart of your thyroid disease. Please remember that your pituitary simply cannot be abnormal in isolation.
Interested in learning more about your thyroid? I would love for you to do some more learning to really discover more about it, and what you can do to preserve the long-term health of your thyroid (and your long-term happiness). Please, take the Thyroid Quiz (Click Here) today.

1. Schedule a Thyroid Second Opinion with me, Dr. C, Click Here for Details
2. Download and use my Favorite Recipes Cookbook Here
3. Check out my podcast Medical Myths, Legends, and Fairytales Here
Dr. Alan Glen Christianson (Dr. C) is a Naturopathic Endocrinologist and the author of The NY Times bestselling Adrenal Reset Diet, The Metabolism Reset Diet and The Thyroid Reset Diet.
Dr. C’s gift for figuring out what really works has helped hundreds of thousands of people reverse thyroid disease, lose weight, diabetes, and regain energy. Learn more about the surprising story that started his quest.


